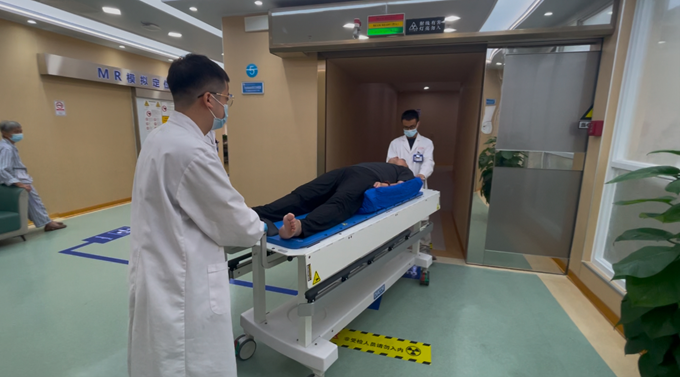
Insights from Medical Physicist Shinobu Kumaga
At Teikyo University Hospital in Tokyo, Japan, the radiation oncology team is continually exploring ways to integrate new technologies that enhance clinical precision while supporting efficient workflows. Medical physicist Shinobu Kumaga, who focuses on treatment planning, quality assurance, and external beam radiation therapy processes, shared the team’s experience implementing the Zephyr patient transfer system into their brachytherapy workflow.
The system was introduced at the hospital in December 2025, making Teikyo one of the early clinical sites in Japan to incorporate this type of integrated transfer technology alongside the Eleka Studio ImagingRing, an advanced, mobile CT scanner. According to Kumaga, the installation was immediately notable for its mechanical stability and consistent performance, helping the team integrate the system into daily clinical routines without adding complexity.
One of the most significant improvements has been in workflow efficiency during brachytherapy procedures. Prior to implementation, patients required multiple transfers between rooms using traditional transfer boards—particularly when moving between applicator placement and CT simulation. These manual transfers required significant staff effort and time and could introduce variability in positioning.
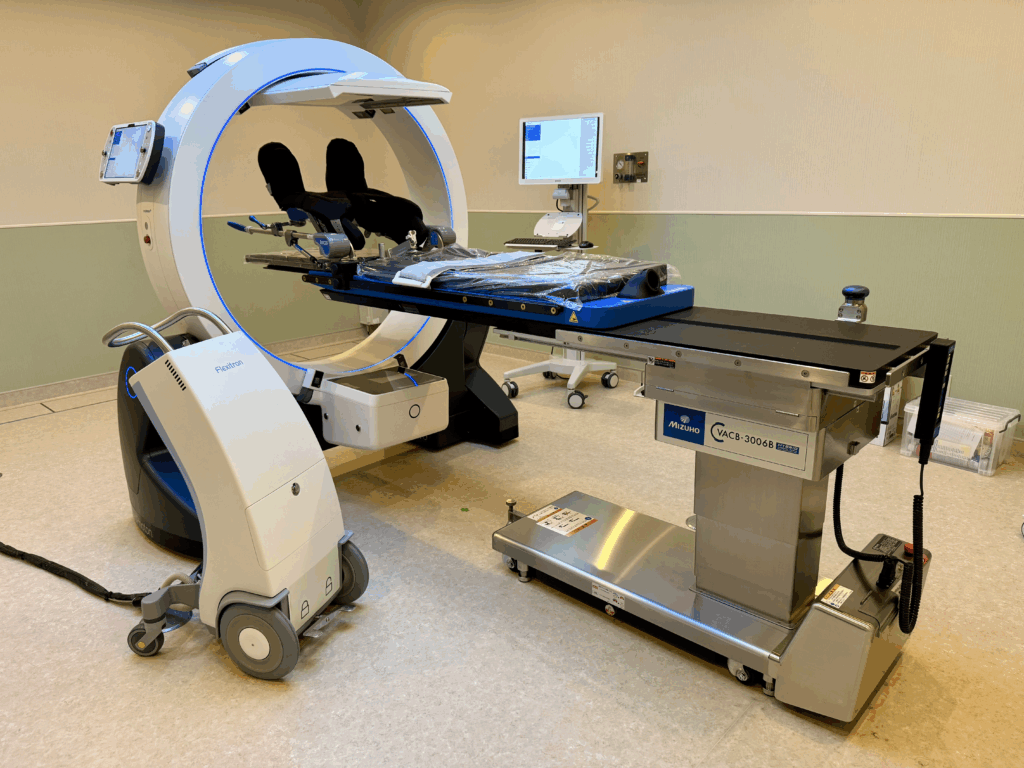 “With the new system, patient movement is greatly reduced,” Kumaga explains. “The patient does not need to be transferred multiple times during treatment preparation.”
“With the new system, patient movement is greatly reduced,” Kumaga explains. “The patient does not need to be transferred multiple times during treatment preparation.”
Reducing transfers has several important clinical advantages. First, it decreases the physical workload on clinical staff, an important consideration for busy radiation therapy departments. It also helps reduce the potential for applicator displacement or positioning variability, which can occur when patients are moved between imaging and treatment environments.
For Kumaga, the biggest benefit is the way the technology supports greater clinical focus and reproducibility. “Every treatment requires precise applicator placement by the physician,” he notes. By minimizing patient movement, the team can concentrate more fully on positioning accuracy and treatment preparation.
Since implementation, the team has treated many cervical cancer patients with the new workflow. Even in these early cases, the technology has helped streamline the process and support a more controlled treatment environment.
Looking ahead, Kumaga sees systems like this as part of a broader evolution in radiation oncology—one where treatment planning, imaging, positioning, and workflow integration work together as a unified process.
“In modern radiation therapy, it’s not only about the treatment plan,” he says. “The workflow, imaging, and patient positioning are all essential parts of the treatment process.”
For the team at Teikyo University Hospital, integrating these elements more seamlessly is helping create a safer, more efficient environment for both patients and clinical staff.